Clinical Exposure
We offer well-rounded clinical and procedural training. Our fellows are trained to perform:
- Amniocentesis
- Cerclage (including Shirodkar and MacDonald procedures)
- Percutaneous umbilical cord sampling / intrauterine transfusion (IUT)
- Dilation and evacuation (first and second trimester)
- Cesarean hysterectomy for placenta accreta spectrum and obstetric hemorrhage
Advanced Procedural Training
Because of our unique patient population, we have a high volume of IUTs and cesarean hysterectomies relative to other centers. Our fellows also gain experience in breech extraction of the second twin and operative vaginal delivery (vacuum and forceps).
Continuity Experience
Fellows jointly staff two high-risk clinics at the University of Utah and South Main Public Health Clinic in their first two years and additionally participate in a variety of faculty clinics to broaden their exposure.
Clinical Autonomy
Our fellows function as independent obstetricians for activities that are within the scope of a general OB/GYN. Our fellows are not ‘PGY-5’ residents or super-chief-residents; rather, they enjoy well-deserved autonomy in procedures and patient management that they have already mastered. Fellows have direct supervision for MFM consultations, management, and procedures.
Experiential Learning
We focus on hands-on ultrasound training and have ultrasound and genetic case conferences moderated by experts. As a referral center for the Intermountain West, our fellows are exposed to a high volume of fetal anomalies and fetal/maternal genetic disorders. Our fellows are mainly based at two large tertiary-care hospitals, both with large regional NICUs. The University of Utah and Intermountain Medical Center both have busy Labor and Delivery units, active diagnostic centers, and ample opportunities for education.
Education
Didactics
A favorable education to service ratio is top priority. Our fellows have protected time for all educational activities.
We have a highly structured didactic schedule that emphasizes faculty participation and highlights several guest speakers annually. Many of our faculty are international experts on particular topics and are actively involved in fellow education.
Some examples of recent didactics include:
- Ultrasound didactics
- Postpartum Hemorrhage
- Complex Contraception
- Mental Health Disorders in Pregnancy
- Neurologic Emergencies
- Maternal Fetal Medicine Transports
- Hypertensive Disorders of Pregnancy
- Dermatoses of Pregnancy
- Endocrine Disorders in Pregnancy
- Obstetric Critical Care
- Insulin Management in the Complex Diabetic Patient
- Lower Urinary Tract Obstruction and the RAFT Study
- Autoimmune Disease in Pregnancy
- Placental Pathology
- Pregnancy in the Fontan Patient
- Complications of Monochorionic Twin Pregnancies
- Perspectives of Care of Fetuses and Infants with Trisomy 13 and 18
- Single Ventricle Physiology
- Inherited Bleeding Disorders of Pregnancy
- Fetal Midline Brain Abnormalities
Our weekly/monthly conferences include the following:
- Fetal Care Conference (weekly)
- MFM Division Research meeting (twice monthly)
- Ultrasound Conference (twice monthly)
- Accreta Conference (monthly)
- Perinatal Pathology (monthly)
- Consensus Conference (6 times per year)
- MFM Didactics (weekly)
- Advanced Congenital Heart Disease Conference (monthly)
- Fellowship in Progress (3 times per year)
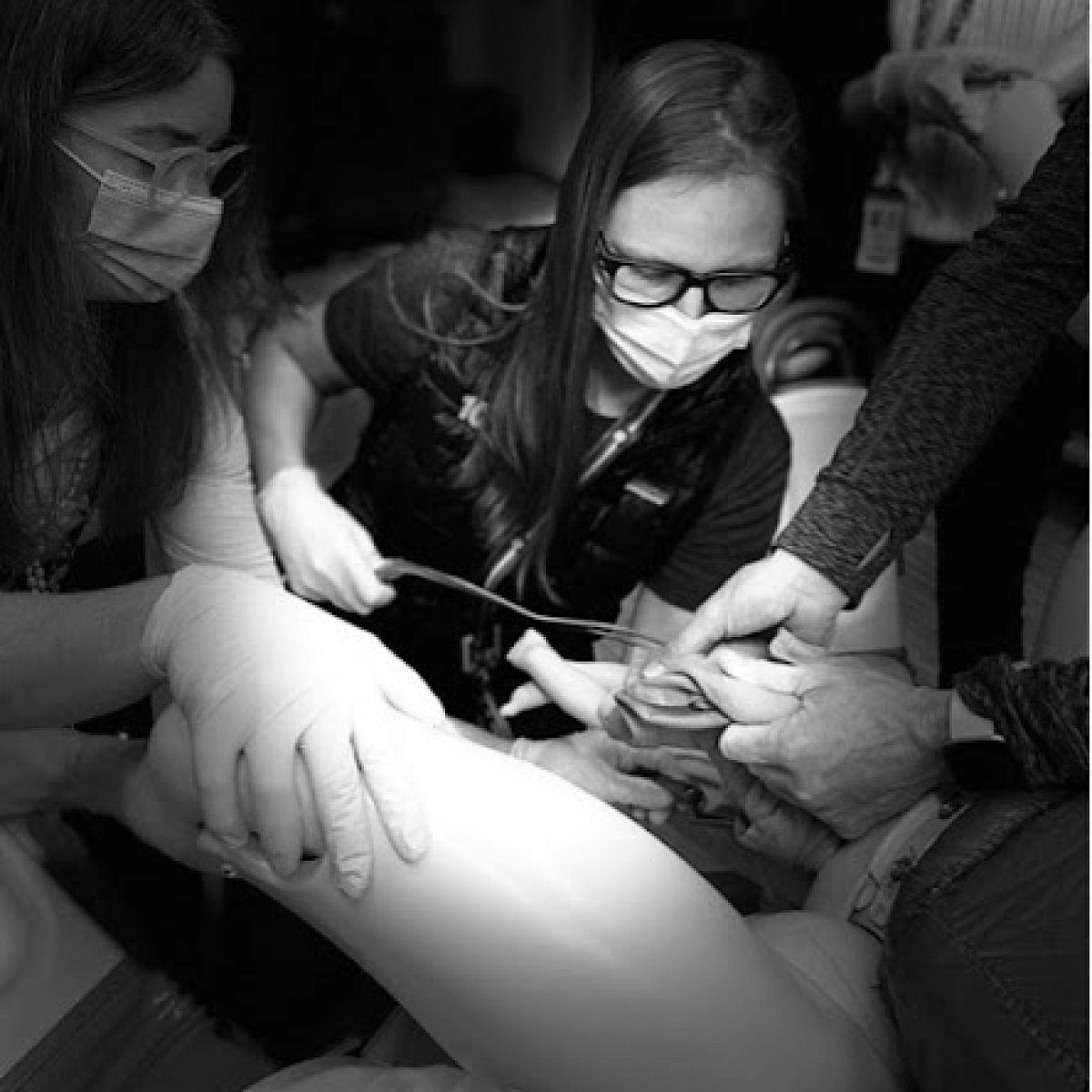
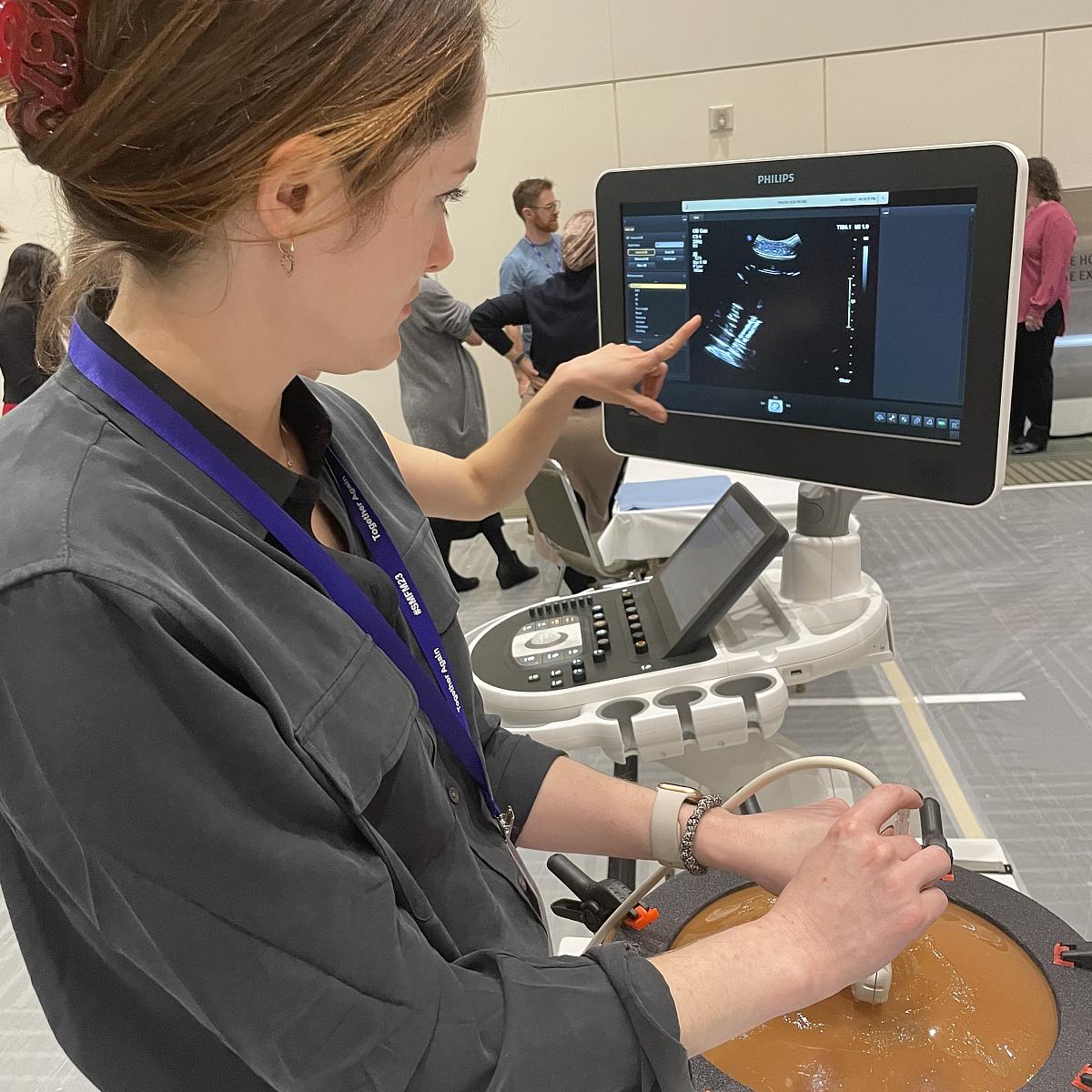
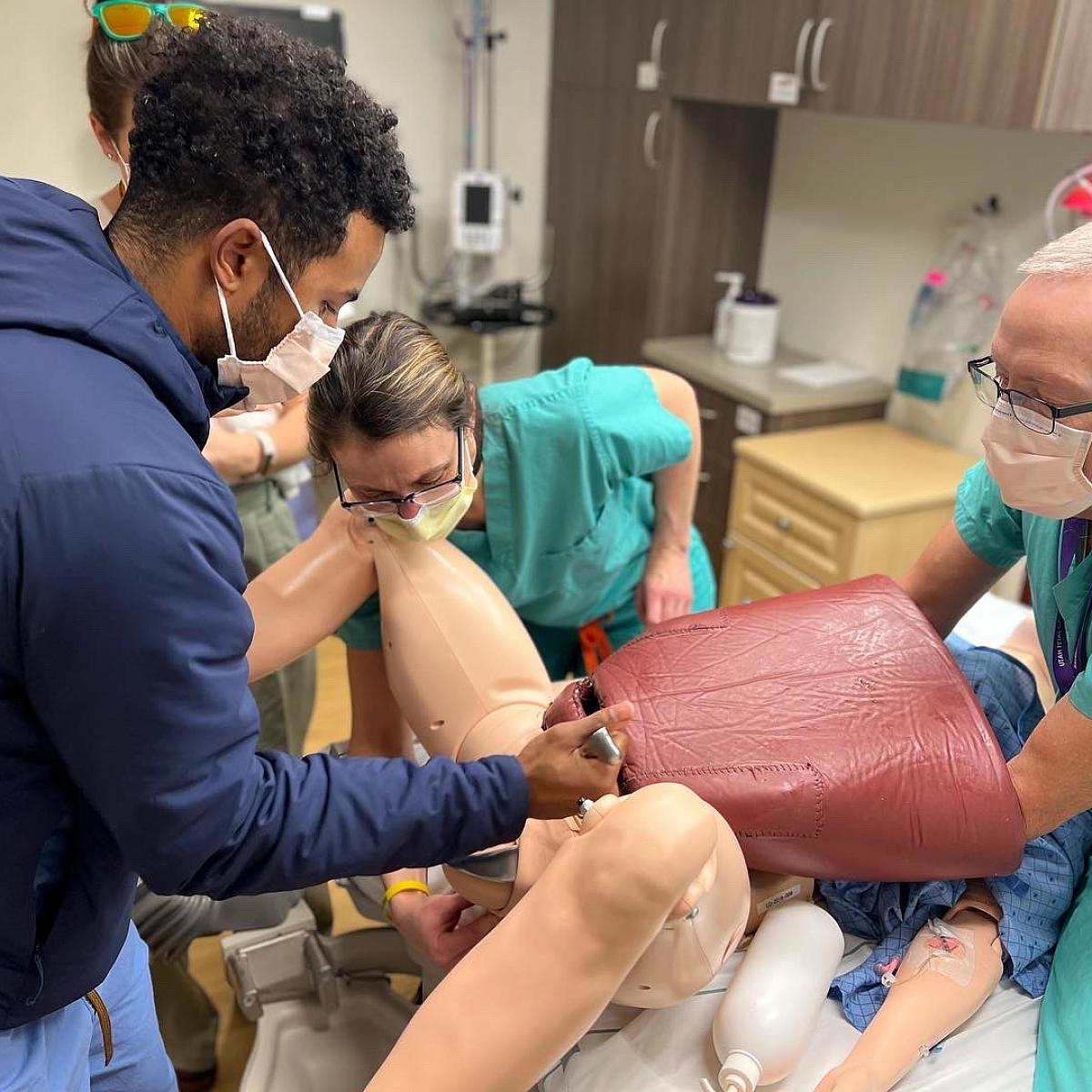
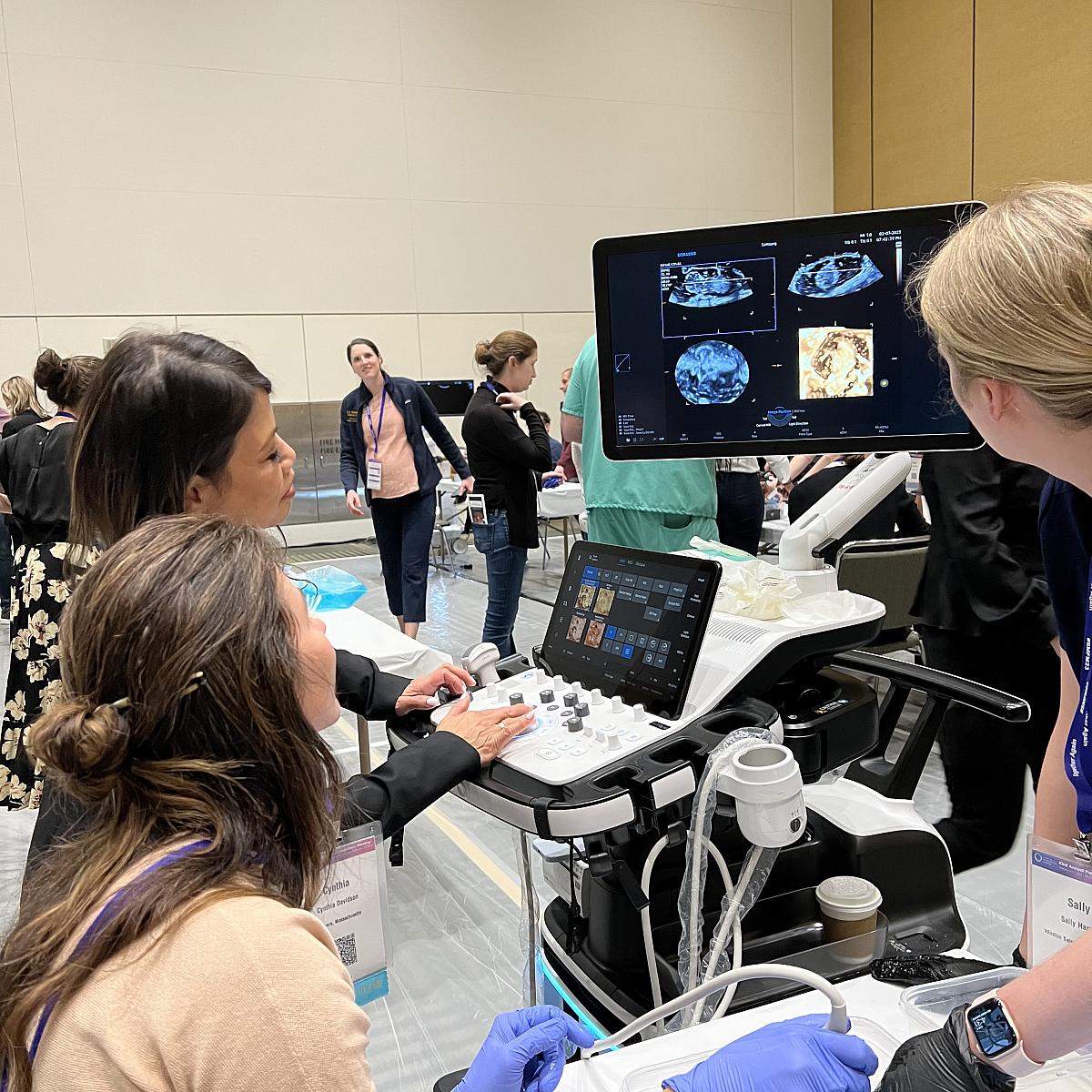
Simulation
We have a successful simulation curriculum (see pictures below), led by Drs. Eller and Richards, that facilitates procedural knowledge and competency.
Our simulation sessions include:
- Difficult deliveries (operative vaginal delivery, cesarean techniques)
- Communication
- Needle Procedures
- Abdominal Packing and OB Salvage Surgery
- Fetal echocardiogram
Ultrasound
Three months of the first year ultrasound experience is dedicated to scanning in addition to routine scheduled didactic lectures. Experience with reading ultrasound begins in the second year and continues throughout fellowship with 6 months of dedicated clinical time. Additional time in our diagnostic center can be scheduled if desired to pursue individual educational goals.
Critical Care
Fellows complete a one-month rotation in the Shock-Trauma ICU at Intermountain Medical Center during the first year of fellowship. Our fellows are an active part of the ICU team (acting as residents) and take call with the ICU team.
Fellows have no MFM obligations during this rotation. Our fellows become familiar with the principles of critical care and are able to apply these skills and knowledge to the obstetric population. Fellows will also be involved in caring for critically ill pregnant/postpartum patients during their obstetric rotations.
Genetics
Our fellows complete the national Basic Training in Reproductive Genetics curriculum during their second year of fellowship (https://mfprecision.ucsf.edu/basic-training/) and work closely with genetic counselors throughout their clinical rotations. These include participation in pediatric genetics clinic and case conference, neonatal genetic consultations and perinatal autopsies, exposure to genetic counseling, and firsthand observation of relevant laboratory assays. We have a board-certified OB MFM geneticist on our primary MFM faculty (Dr. Byrne) who our fellows have the opportunity to learn from and work with clinically.
Cardiology: Fetal and Maternal Congenital Cardiac Disease
During the second year of fellowship, our fellows complete a one-month pediatric cardiology rotation at Primary Children’s Medical Center.
This rotation provides additional training in sonographic evaluation of the fetal heart and is designed to improve diagnostic skills for fetal congenital cardiac disorders. Fellows also participate in adult clinics to improve knowledge and competence in the obstetric care of women with congenital heart disease.
Fellows also have the opportunity to obtain their fetal echo certification.
Customizing Our Curriculum to Meet Fellows’ Needs
We work with our fellows to customize their educational curriculum and meet their unique needs through both internal and external rotations, in the US and abroad.
If you have a particular area of interest that is not covered in-depth by our current curriculum, talk with us about ways we might be able to tailor your educational experience.