Research & Innovation

Research & Innovation
Friend or Foe—IDH1 mutations in Glioma
Somatic heterozygous IDH1 mutations occur in >70% of the lower-grade gliomas and secondary glioblastomas. Interestingly, patients with IDH1 mutations have a median overall survival 2—3 times longer than those without, and yet these patients ultimately succumb to the malignancy despitethe best treatment currently available.
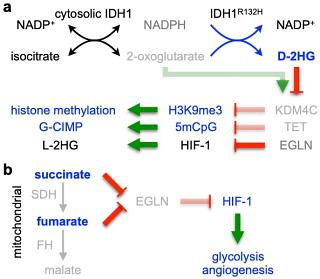
IDH1 encodes the cytosolic isocitrate dehydrogenase 1 that converts isocitrate and NADP+ to 2-oxoglutarate and NADPH. The mutant enzyme acquires a neomorphic activity that converts further the products of wild-type IDH1 to D-2-hydroxyglutarate (D-2HG), a potent inhibitor of 2-oxoglutarate-dependent histone demethylases and 5-methylcytosine hydroxylases. Consequently, gliomas with IDH1 mutations exhibit histone and DNA hypermethylation. IDH1 mutation is widely believed to be oncogenic for glioma genesis and progression through epigenetic and metabolic reprogramming. Accordingly, drugs targeting mutant IDH1 have been developed and are highly effective in blocking D-2HG production.
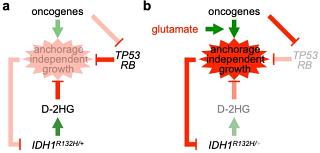
While the efficacy of ongoing clinical trials remains to be seen, we caution counterproductive outcomes as a result. We have proposed a counterintuitive hypothesis that heterozygous IDH1 mutation is intrinsically tumor suppressive and beneficial to the patient; the tumor-suppressive activity, however, is undermined by various intracellular and extracellular factors, notably the neurotransmitter glutamate—abundant in the frontal lobe—as well as inactivation of tumor-suppressor genes (TP53 and ATRX), selection against IDH1 heterozygosity, and reducing equivalents. This dynamic hypothesis not only provides an explanation for the genetic preservation of IDH1 mutations throughout glioma development and progression but also accounts for the prevalence of IDH1 mutations specifically in glioma and the beneficial effect to these patients. Currently, we are studying these undermining mechanisms that drive glioma progression in order to identify effective therapeutic targets.
Glioma Metabolism and Hypoxia
Metabolic reprogramming is an adaptive response critical for the survival and proliferation of cancer cells through the reduction of glucose oxidation (the Warburg effect) and diversion of glycolytic metabolites for the synthesis of macromolecules. The mitochondrial pyruvate carrier (MPC) protein complex, consisting of MPC1 and MPC2, is essential for pyruvate transport into mitochondria. In most human cancers, MPC1 is frequently deleted or down-regulated and, furthermore, the MPC activity is low. The role of MPC in malignant glioma, however, seems more complex, as indicated by our bioinformatics analysis of patient data and experimental data. We hypothesize the cerebral cortex provides a unique microenvironment for tumor cell survival and we are actively testing this hypothesis in order to identify metabolic vulnerabilities of glioma cells that can be used for therapeutic intervention.
Previous studies from my lab and others have indicated a critical role for hypoxia (low oxygen tension) in malignant progression. We first demonstrated in cell culture models that the hypoxia-inducible factor 1α (HIF-1α), a master regulator of oxygen homeostasis, induces genetic alterations by inhibiting DNA repair. At the molecular level, we identified a novel mechanism that accounts for the hypoxic suppression of DNA repair via the Myc pathway. To demonstrate in vivo effects of HIF-1α on genetic alteration, we are employing mouse genetic models to test our hypothesis that HIF-1α drives glioma progression by inducing genetic alteration.