About Us
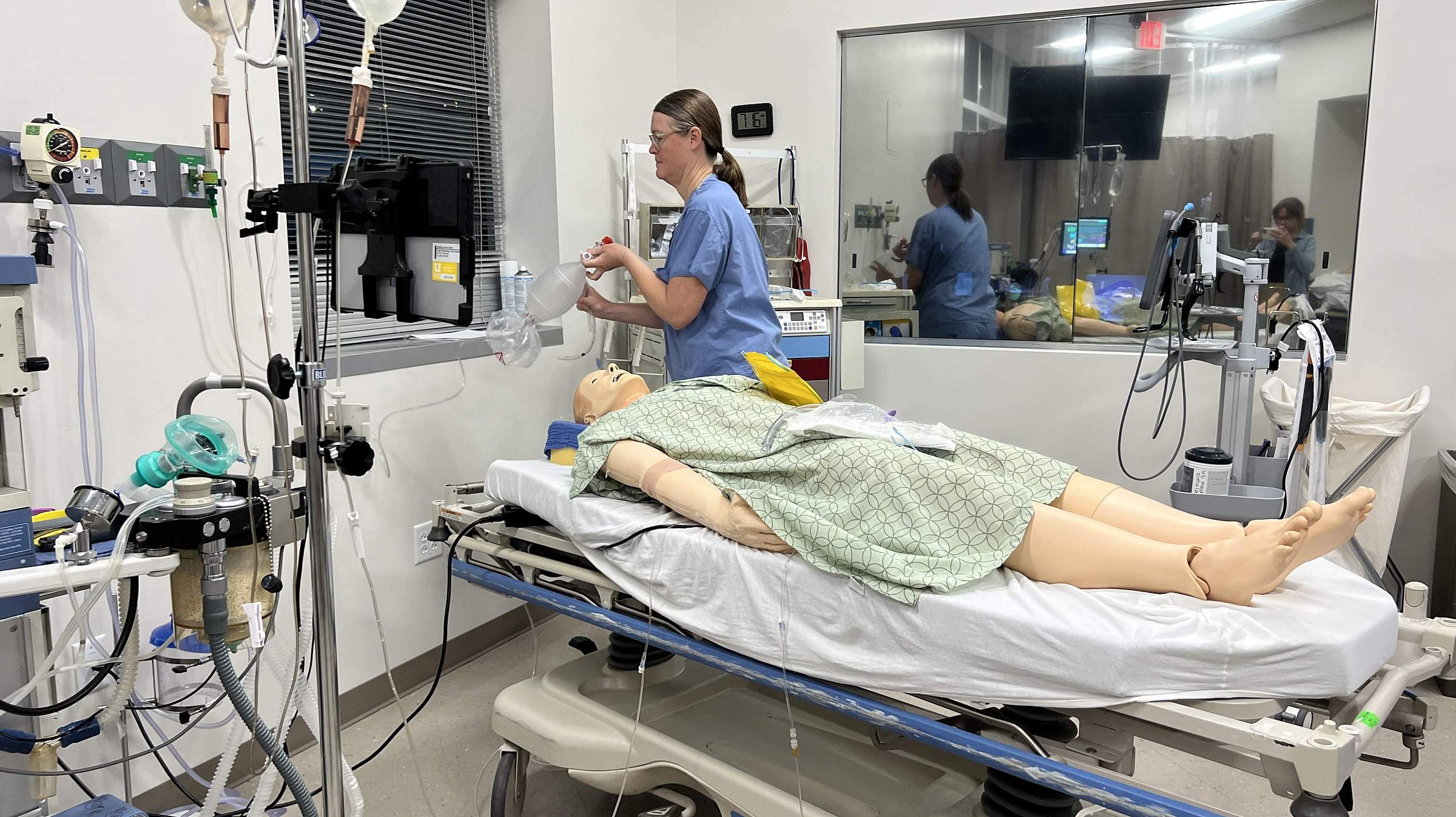
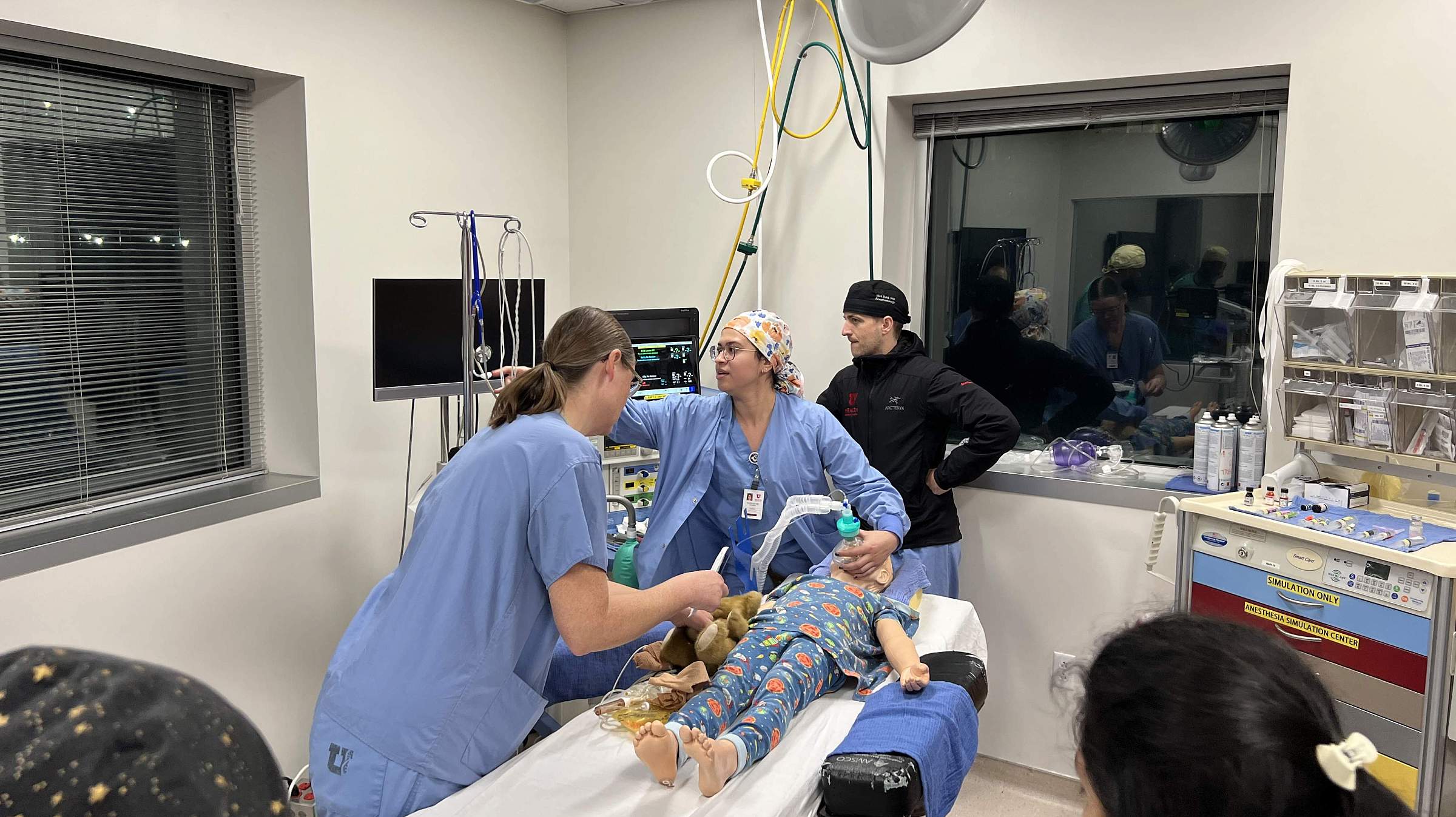
The Center for Patient Simulation at the University of Utah provides cutting-edge, high-fidelity training for healthcare professionals, researchers, and industry partners. While housed within the Department of Anesthesiology, our facility serves all departments and schools across the university, as well as external organizations, including medical device manufacturers and leading healthcare institutions.
Our simulation center offers a realistic clinical environment equipped with advanced patient simulators, customizable training spaces, and state-of-the-art audiovisual capabilities. Whether supporting medical education, conducting research, or facilitating usability studies, we provide tailored solutions to enhance learning, improve patient safety, and advance healthcare innovation.
Located within University of Utah Health, we are dedicated to collaboration and excellence in simulation-based training. Explore how our facilities can support your educational and professional needs.
Key Milestones in Simulation Excellence
Moved to Building 379 in preparation for the new School of Medicine, expanding simulation capabilities with a state-of-the-art operating room and ICU.
Developed COVID-19 simulation training for anesthesiologists, CRNAs, and technicians, adapting education materials to pandemic needs.
Joined the Theodore H. Stanley Annual Update in Anesthesiology Conference, providing hands-on difficult airway workshops for attendees.
Partnered with U of U Trauma Services to deliver in-situ trauma simulations, integrating anesthesiologists, surgeons, nurses, and EMTs.
Added a North Wing with an ICU simulation area and launched a Central Line Placement Course for anesthesia, surgery, and trauma residents.
Became one of the first American Society of Anesthesiologists (ASA)-endorsed MOCA simulation centers in the western U.S., offering Maintenance of Certification in Anesthesia (MOCA) courses.
Began conducting usability studies for medical device companies, establishing partnerships with major manufacturers.
Relocated to a new space on the 3rd floor of the School of Medicine, featuring a simulated operating room and debriefing room near the hospital ORs.
Founded in the basement of the U of U School of Medicine, the center began training medical students and anesthesia residents using high-fidelity simulation.