 |
| Darla Rogers and her husband Tim at the Huntsman Cancer Institute, three years after her stage IV colon cancer diagnosis, happy and upbeat thanks in part to the interventional radiology treatment known as Y-90 radioembolization. |
By Michael Mozdy
It was Mother’s Day 2014, and Darla Rogers’ celebration wasn’t going as planned. As the day wore on, some lower stomach pain had become unbearable, and her husband Tim insisted they go to the local ER. They feared appendicitis, but the source of the pain proved to be much more serious.
The doctor came back with her CAT scan results crestfallen. He cut to the chase: “I’m sorry, Darla, you have stage IV colon cancer,” he reported. “There’s nothing I can do for you – you’re going to die.”
Darla was stunned and profoundly sad. She and Tim had just embarked on a new phase of their lives, having gotten married just six months ago. They both had kids and grandkids, and were looking forward to many happy years ahead.
She remembers one other thing from that day. The oncologist who explained her recommended chemotherapy and left her with these words: “Darla, you need to fight for your life.”
How to Fight Metastatic Liver Tumors
Colorectal cancer is frightening enough, but “stage IV cancer” means that it has spread – or metastasized – to other parts of the body. In Darla’s case, the cancer had spread to her liver and her lungs. The liver, in particular, is a cause for concern; it’s the largest organ in the body, responsible for many essential enzymatic processes, and it’s impossible to live without a functioning liver.
 |
| Darla's oncologist, Glynn Gilcrease, III, MD. |
Despite the first words she heard when she received her diagnosis, it turns out there was something that could be done for Darla. She switched hospitals to the Huntsman Cancer Hospital and started an aggressive chemotherapy regime under the care of Glynn Gilcrease, III, MD, Associate Professor in Oncology. Darla had a difficult time tolerating the chemo for 6 months, at which point Gilcrease switched her to maintenance chemotherapy.
The large amount of cancer in her liver concerned Gilcrease. “It’s a very common site for metastatic colon cancer,” he explains, “but it can hold a large bulk of the disease, which can create pain and fatigue and greatly lower someone’s overall quality of life. If we can control the amount of cancer someone has, they would have virtually no symptoms.”
Gilcrease is a close colleague of Ryan O’Hara, MD, the section chief for Interventional Radiology. They discussed Darla’s case. “We spoke at several points about the right time to do liver-directed therapy,” Gilcrease recalls. “Because we had such good control of her primary tumor due to chemo and she was weary of continuing on maintenance chemo, we felt that about 9 months into her maintenance chemo was a good time for a different treatment.”
O’Hara would perform radioembolization, a technique that delivers millions of tiny radioactive beads through the bloodstream to the liver where they lodge themselves and irradiate the tumors directly.
 |
| Darla's interventional radiologist, Ryan O'Hara, MD, section chief of Interventional Radiology |
O’Hara and the six other interventional radiologists in his section specialize in non-invasive, image-guided techniques to perform what are traditionally thought of as surgical procedures like biopsies, drains, stent placements, and more. Interventional radiologists are masters at performing procedures with the most difficult of patients – people who couldn’t survive traditional surgery, for instance. In addition to their skills navigating delicate anatomy with nothing but catheters and fluoroscopy imaging, they are known for their ability to improvise when faced with the unexpected, whether it be collapsing arteries, difficult anatomy, or any number of co-morbidities.
For Darla, O’Hara chose a product called SIR-Spheres made by the company Sirtex, which are microspheres infused with a radioactive isotope called Yttrium-90, or Y-90. This radioactive isotope is a by-product of the uranium in nuclear reactors, and its properties make it very useful medically. Y-90 emits beta-ray radiation, which travels a shorter distance than gamma rays or x-rays, and the SIR-Spheres only emit radiation for about 10 days.
The other important property of these microspheres is their size: just 30 microns (millionth of a meter) in diameter. This makes them about 1/3 the width of a human hair, or just four times bigger than a red blood cell. This tiny size allows them to travel through arteries right to the tumor, but they get stuck as the artery turns into very small capillaries on the surface of the tumor. This accomplishes two things: 1. it slows the flow of blood feeding the tumor, and 2. it disperses the microspheres over the tumor so that the radiation emitted has the best chance of shrinking or destroying it.
Darla’s Journey
O’Hara was careful to ensure that Darla’s body would tolerate the treatment. First, Darla had what’s called a mapping angiogram of her hepatic artery. O’Hara threaded a catheter through an artery in her groin to the hepatic artery feeding the tumors on her liver. This allowed him to examine how blood flows to her liver and see if the pathway was sufficient for the treatment.
After this, he checked how well the liver could be targeted without affecting other organs. He temporarily closed off other arteries where he didn’t want the radiation to go and injected a harmless “tracer agent.” Darla then received a nuclear imaging scan to see how much of the tracer agent stayed in her liver and how much traveled to other organs like the lungs.
All signs were positive, so O’Hara ordered a specific dose of SIR-Spheres for Darla according to her unique biology and amount of liver tumors. A few weeks later, in about a 90-minute procedure, O’Hara used those same techniques to deliver the radioactive microspheres to Darla’s liver tumors.
Darla doesn’t mince words when describing how her body reacted to the Y-90: “It felt like my insides were melting,” she admits. For most people, including the ones in her stage IV colon cancer survivor support group, Y-90 microspheres cause minimal side effects. But Darla was an outlier. She had a tough 8 days of discomfort until one day she woke up and knew she had turned a corner.
“It seemed like I was getting better every day,” she reports. She felt better than she had in a long time. Gilcrease decided she could handle surgery to remove the tumor in her colon, and they successfully removed a foot of her bowel along with a large tumor. The metastatic tumors on her liver and in her lungs went away and she took a long “chemo holiday” for two years. To Darla, it felt like a miracle.
“Chemo holidays are usually 3-6 months,” explains Gilcrease. “It’s quite rare to see a patient have such a long time without chemo, especially with active metastatic disease in the liver. Having treated quite a few patients, I think that it’s certain Y-90 helped her quite a bit.” One of the things Gilcrease and O’Hara like about Y-90 treatments is that they concentrate on the dangerous and stubborn liver tumors, enabling other types of healing to take place.
Darla’s is not an isolated case. Studies have shown that, for patients with liver metastasis, Y-90 combined with systemic chemotherapy can help to control the disease better than with chemotherapy alone.
Living With Cancer
Last year, Darla was introduced to Suzanne Lindley, a 19-year stage IV colon cancer survivor in Darla’s home state of Texas. Lindley is the cofounder of the support group Yes! Beat Liver Tumors! and as Darla relates, “she took me under her wing and I became one of her poster children.” Lindley organizes fund raisers, retreats, and other events, and before she knew it, Darla’s schedule included a whirlwind three months where she was invited to the People’s Choice Awards, to be a model for Fashion Week in New York City, and to attend the Oscars.
Yet cancer survivors must always face the possibility of the cancer returning, and that’s exactly what happened to Darla. Her cancer had returned to her lungs, liver and peritoneum. Her care team scheduled a new round of chemotherapy and two Y-90 treatments, and in late summer 2017, Darla was back at the Huntsman Cancer Center.
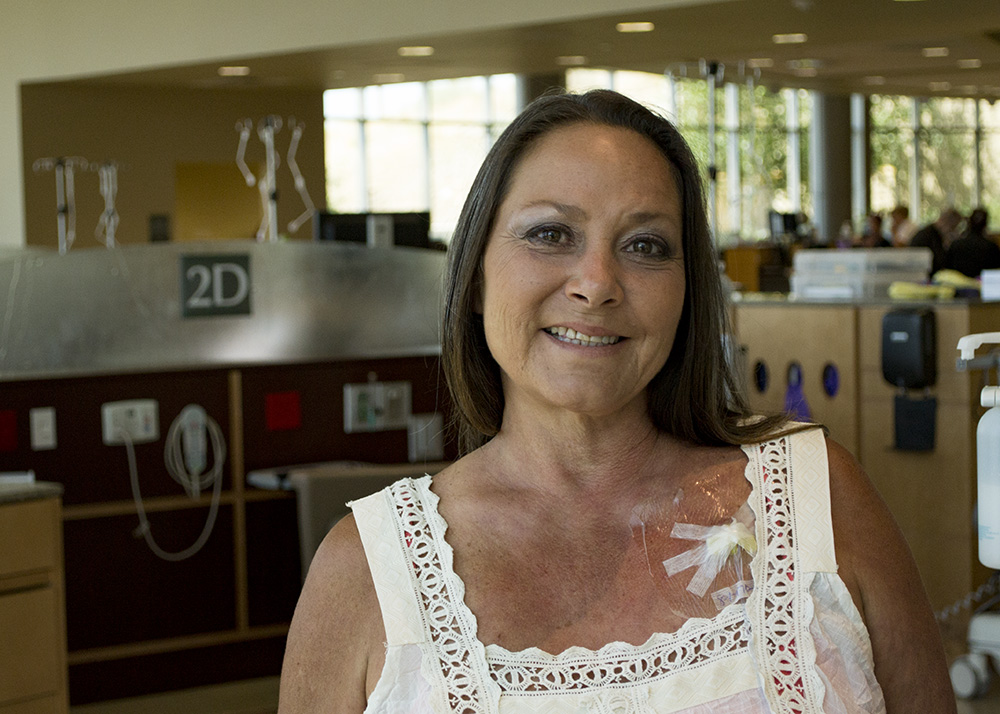 |
| Darla in the Huntsman Cancer Hospital Infusion Center. Photo: Michael Mozdy. |
In August 2017, Darla spoke with me while receiving her chemotherapy in the Infusion Center at Huntsman Cancer Hospital. She and her husband, Tim, drive down from their home in Mountain Green for the treatments. She was comfortable with herself, smiling, and unrelentingly optimistic. As Tim stood off to the side, she gushed about him.
“Tim is a rock and I wouldn’t be here without him. When we were told we should do the Y-90 again, I cried all the way home, but then we thought another 2 years, and how fabulous would that be?”
She suffered a longer two-week post-embolization syndrome on her third Y-90 treatment, but still she attests to its power. “Once again, the mighty Y-90,” she laughs. “Once you get past that initial period, every day, every hour you feel better and better. I feel like a million dollars now – no pain and my energy level has come back.”
When asked about her brush with fame as an Oscar attendee and New York City runway model, she shrugs it off. “What’s more fun for me is camping with my husband. He builds me little teardrop campers. The first one was called Snuggle Shack, the next one was Happy Shack, and he’s building Hope Shack right now.” Tim’s hobby gives him time to recharge as a caregiver and it gives them both something to use to enjoy life together. They’ve traveled all across the country with their teardrop campers, from visiting grandchildren in Georgia to exploring Washington state.
 |
| Darla and Tim’s custom teardrop camper. Photos: Darla Rogers. |
They’ve also been able to have fun with their dream home in Mountain Green. They’ve put in a 25-foot waterfall that ends in a stone- and flower-encircled pond. They have fruit trees, a big garden, two German Shepherds, and this year Darla planted 135 pots of petunias. She sees her children at least once a month and glows when she talks about her grandkids, especially when they play in the pond and become “mudpie grandcuties.”
 |
| Darla’s pond and flowers, one of her dogs, and she and Tim in Hawaii last year. Photos: Darla Rogers. |
It’s a wonderful life that Darla will always fight for – just as her oncologist told her to do on that difficult Mother’s Day three years ago. Y-90 has been a powerful ally, helping her be not just a cancer survivor but a grandmother, wife, world traveler, fashion model, and constant inspiration to others. “Perhaps the best part of Darla’s story is how high of a quality of life she’s been able to have while on her chemo holiday,” says Gilcrease.
“The Y-90 makes me feel better than the chemo does. I’ll do it as many times as they want me to do it,” she declares. “I’ve had it three times now – I’ll do three more! We just hope for three months at a time… do the scans, and carry on.”
That’s what interventional radiology is all about – helping patients live longer and happier lives through innovative techniques and technologies. O’Hara has doubled the size of this team to seven, each physician bringing specific expertise to the department. They also offer a new Interventional Radiology residency, for those who want to specialize in this challenging and expanding field.
O’Hara sees interventional radiology continuing to push the boundaries of what is considered possible in patient care. “New technologies and techniques emerge every year,” he declares, “and the future has never looked as optimistic for so many patients.”